What Is Fungal Acne (Malassezia Folliculitis)?
Medical review by Danica Alexander, DO
Have itchy acne? If pimple-fighting products do nothing to tame it — or even make it worse — it may be because you don’t have true acne at all but something entirely different. One possibility is fungal acne, also called Malassezia folliculitis or Pityrosporum folliculitis. It can look so much like acne that it’s often misdiagnosed. If you’ve been battling small red bumps on your skin for months or even years with no success, read on to learn if fungal acne could be the real cause and if so, how to treat it.
What Is Fungal Acne?
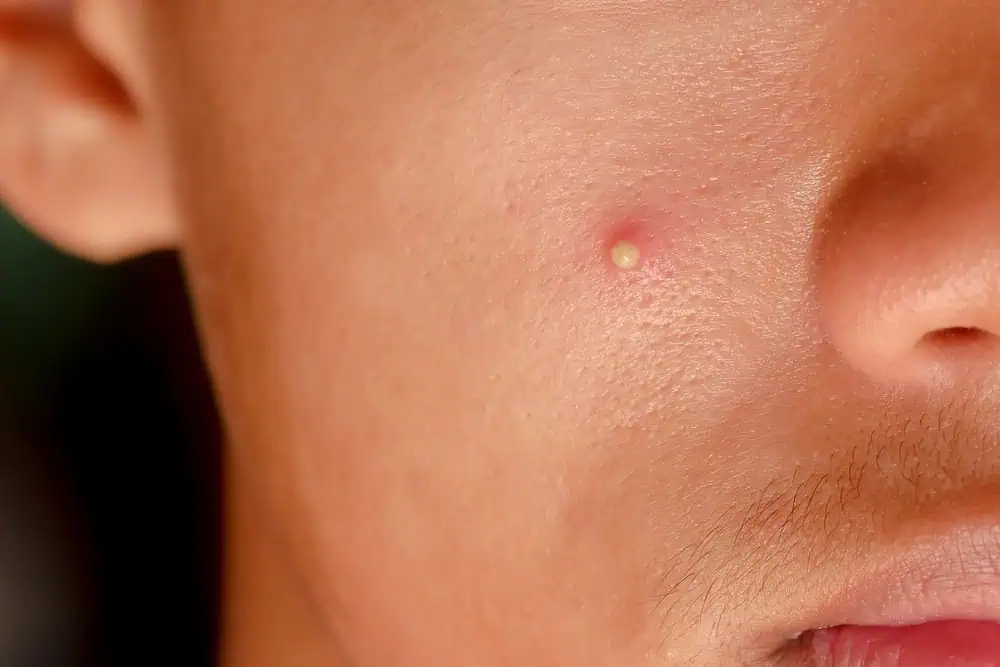
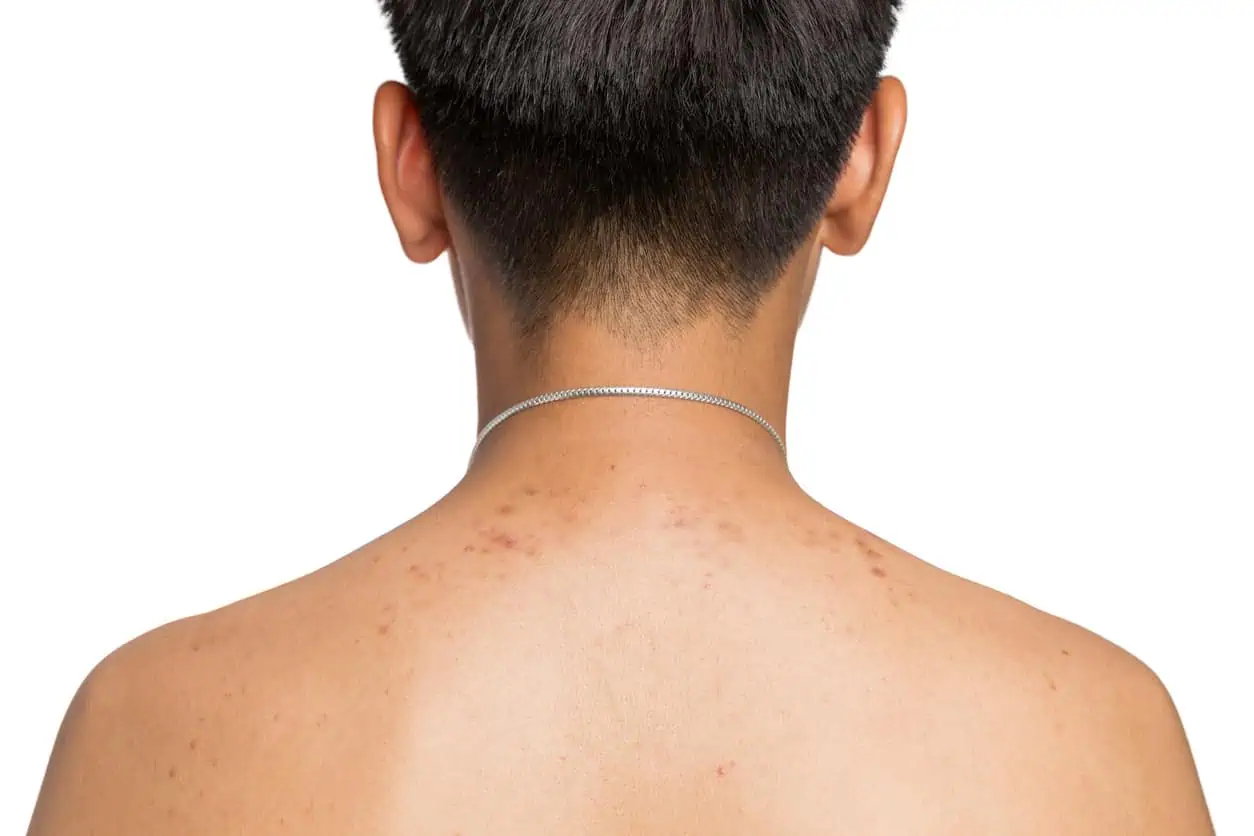
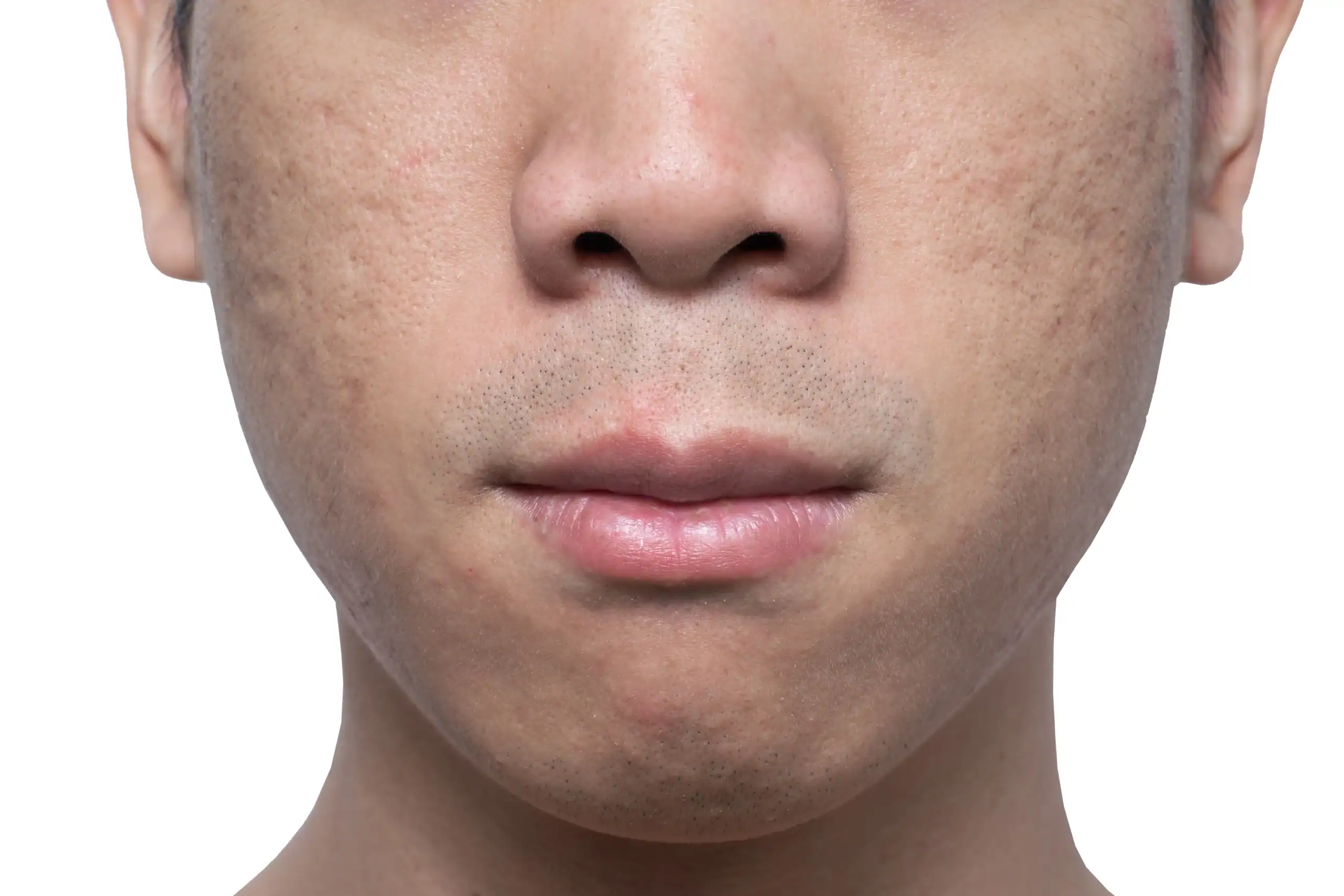
Technically, fungal acne isn’t acne. Acne vulgaris is caused by clogged pores and bacteria. Fungal acne is caused by an overgrowth of a yeast (a type of fungus) that lives on the skin. When this yeast, called Malassezia, invades the hair follicles, clusters of small red bumps can develop. Something these “fungal pimples” fill with yellow or white pus. Itching is a common fungal acne symptom, occurring in about 80% of cases.
Fungal acne on the face may appear on the forehead, cheeks or elsewhere. Fungal acne on the forehead looks like forehead bumps that may line up in rows. The infection can also be seen on the chest, back and arms.
Bacterial Acne vs. Fungal Acne
Fungal acne and acne vulgaris can look alike, so it’s not uncommon to think you have true acne when fungus is to blame. (To complicate matters, some people have both.) But there are a few telltale differences. A Malassezia infection is much more likely to itch. The bumps are smaller and more uniform in size, and they tend to appear in clusters.
If you have another skin condition caused by an overgrowth of yeast, such as seborrheic dermatitis (dandruff), you’re more likely to have fungal acne.
Who Gets It?
Anyone can develop this type of acne, but it’s more common in teenagers and young men. Other risk factors include:
- Having oily skin
- Sweating a lot or living in a hot, humid environment
- Wearing tight clothing or clothing that doesn’t breathe
- Re-wearing sweaty clothes or staying in sweaty clothing for too long
- Wearing heavy makeup
- Taking certain medications, such as oral contraceptives, antibiotics, oral steroids and immunosuppressive drugs
- Having a disease such as diabetes, leukemia or lymphoma that increases the risk of yeast overgrowth
How To Get Rid of Fungal Acne
A dermatologist can determine whether you have acne and which type. Getting an accurate diagnosis is critical before starting fungal acne treatment.
Your dermatologist may recommend an over-the-counter topical antifungal medication or prescribe a stronger version. If it doesn’t do the trick, you may need a prescription oral antifungal. These folliculitis medications sometimes work better than topical products, and they work fast, but they can cause side effects such as stomach pain and diarrhea.
If antifungal medication can’t cure your Malassezia folliculitis, your dermatologist might recommend photodynamic therapy. It uses light energy in combination with a drug activated by light to kill the fungus.
Paying close attention to your hygiene is an essential part of treating and preventing a Malassezia overgrowth. Shower regularly, especially after you’ve been sweating, and wear loose, breathable clothing. Don’t use oily creams. If you’ve had more than one bout of fungal acne, try washing the affected area(s) with anti-dandruff shampoo.
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Is It Bad to Pop Pimples? (And How Else to Get Rid of Acne)
Medical review by Tia Bean, MSN, APRN
Pimple popping is having its day. In fact, it’s become a spectator sport. Videos featuring close-ups of whiteheads erupting like Lilliputian volcanoes under pressure from an extractor tool or (sometimes ungloved) fingers get millions of views on YouTube and TikTok. Blackhead popping and cyst popping videos draw plenty of eyeballs, too. But is it bad to pop pimples?
When asked, “Should you pop pimples?”, most dermatologists firmly say no. You might think it will help the pimple heal faster, but the experts note that pimple popping at home probably won’t help and may hurt.
5 perils of popping pimples
DIY pimple popping is a bad idea for at least five reasons:
- Pressing on and squeezing an acne blemish can push the oil, dirt and bacteria that’s clogging the pore deeper into your skin and make your acne worse. If the crud gets deep enough, nodules or painful cysts can form. Cystic acne is especially hard to treat and likely to lead to scars.
- Dirt, bacteria and oils can travel from your fingers into your pores and nearby hair follicles.
- The opening left behind after you pop a pimple could turn into an acne scar.
- The pressure you put on your skin could lead to a small, possibly permanent spider vein on your face.
- If you really go to town on a blemish, the force can cause the skin to tear enough to create an open wound that can bleed, scab over and scar, as well as open the door to infection.
What to do instead of pimple popping
Just because it’s unwise to pop a pimple doesn’t mean you’re entirely at its mercy. If you leave it alone, it will go away on its own, typically within three to seven days unless it’s a deep cyst. But if you want to help it along, you have some safe options. Here’s how to get rid of acne faster according to the American Academy of Dermatology:
- Turn up the heat on whiteheads. A warm compress can help coax a pus-filled pimple along. Soak a clean washcloth in hot water, wring it out and apply it to the area for 10 to 15 minutes three or four times a day.
- Put it on ice. To ease pain and inflammation from a pimple deep in the skin, wrap an ice cube in a clean washcloth or paper towel and apply it for 5 to 10 minutes. Repeat after a 10-minute break.
- Battle bacteria with benzoyl. Dabbing on a 2% benzoyl peroxide product once or twice a day will help dry up pimples and prevent infection.
Acne extraction and more: What a dermatology provider can do
Is it bad to pop pimples? At home, yes—but your dermatologist may be able to do it safely. For stubborn zits or times when you need to get rid of a pimple fast for a special event, a dermatology provider can use one of several techniques depending on the size and type of blemish:
- Acne extraction. Acne extraction is performed with sterile instruments designed for this purpose to safely remove blackheads and whiteheads.
- A corticosteroid injection. Injecting a corticosteroid into a large, deep pimple or a painful cyst reduces inflammation and starts to shrink the breakout within 24 to 72 hours. Shrinking the blemish in this way can reduce the chances of scarring. Corticosteroid injections are typically used for single cysts or nodules, not multiple zits.
- Incision and drainage. If you have a particularly large cyst or nodule, the dermatology provider can open it using a sterile needle or surgical blade and then clean out the contents.
Pimple popping can be hard to resist, but treating a bothersome breakout is best left to a professional. A dermatology provider can also develop an acne treatment plan to keep pimples and other blemishes from forming in the first place. Learn when to seek a dermatologist’s care for acne vs. trying to treat it at home.
Ready to make an appointment for acne treatment? Schedule one today.
Written by Maura Rhodes, a New Jersey-based writer and editor specializing in health and well-being.
Dairy and Acne: Is There a Link?
Medical review by John Minni, DO
Does dairy cause acne? Claims of a relationship between diet and acne have circulated for decades. Depending on what you read, you may think dairy products are among the worst offenders. But what’s the reality when it comes to dairy and acne? Should you give up pizza, milkshakes or lattes for clearer skin?
Little research has been done to investigate a possible connection between dairy and acne, and some results of published studies have been pointed to opposite conclusions. What’s more, different types of dairy appear to have different effects. If the question is “Can milk cause acne?” the answer is a qualified maybe.
“Acne is a complex condition with many causes, including genetics and hormones,” said John Minni, DO, a board-certified dermatologist at Water’s Edge Dermatology. “Certain foods may contribute to acne in some people, but they won’t cause acne if you aren’t already acne prone.”
Milk and acne
If any dairy product contributes to acne — and that’s still an “if”— it’s milk. Ironically, according to at least one study, skim milk and low-fat milk may be more likely to trigger breakouts than whole milk.
If you have acne-prone skin, go ahead and eat cheese. Research has not found a connection between cheese and acne (though you may want to limit cheeses that are rich in saturated fat for other health reasons). As far as yogurt goes, spoon it up.
“Yogurt that contains probiotics might actually improve acne by reducing inflammation in the body, and potentially, by keeping the bacteria associated with acne in check,” said Dr. Minni.
Are the hormones in cow’s milk to blame?
All cow’s milk contains natural hormones. Most milk that isn’t organic also contains artificial hormones that are given to the cows to boost milk production.
In humans, hormonal changes that come with puberty, menstruation and stress can cause acne flare-ups. It’s possible that the hormones in cow’s milk could also cause flare-ups by throwing off the balance of hormones in your body.
One culprit may be insulin-like growth factor-1 (IGF-1), which is thought to trigger breakouts in humans. Cows produce it naturally, and the synthetic hormones given to cows makes them produce more of it.
In addition to IGF-1, various androgens — sex hormones sometimes called “male hormones,” even though females have them too — could also play a role. Testosterone, for example, causes a reaction in the body that stimulates the sebaceous glands to produce more pore-clogging sebum.
Milk and inflammation
Some people suspect that milk may worsen acne by increasing levels of inflammation in the body.
“We now know that inflammation is a major factor in acne,” said Dr. Minni. “In fact, acne is considered an inflammatory disease.”
It’s not clear how, or whether, milk inflames the body. One popular theory is that the sugar in milk boosts inflammation by spiking blood sugar and insulin levels. This might explain why skim milk appears to be more likely than whole milk to cause acne in acne-prone skin. The fat in whole milk lowers its glycemic index (though only slightly), which means slightly lower blood sugar spikes.
Milk may be more likely to cause inflammation if you consume a lot of it or you’re allergic to one of its components.
Time to give up milk?
Banning milk from your diet won’t eliminate your acne for good because it has no effect on underlying factors such as genetics. And think of your bones: They need calcium, and for many people, milk is a key dietary source. Before you give up milk, talk with a registered dietician about how to get enough calcium from other sources.
Also talk to your skin care provider about what’s causing your acne. Chances are, there are other reasons for it. Milk may be low on the list if it’s on the list at all.
How to drink milk without getting acne
If you think milk might be contributing to your breakouts, giving up milk may not be necessary. Try these measures first.
- Scale back your consumption. In one study, the more milk people drank, the stronger the acne connection was.
- Switch to whole milk.
- Buy organic.
Whatever changes you make, give them time to work. A dietary shift could take weeks or months to have a noticeable effect. And keep your expectations in check. “Most cases of acne don’t magically disappear after cutting out a food,” said Dr. Minni.
Your best bet: Work with your skin care provider, who can prescribe effective acne medication and recommend a pimple-fighting skin care routine that’s right for your skin.
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
How to Get Rid of Back Acne
Medical review by John Minni, DO
Back acne, or “bacne,” can be a major summer bummer. In the winter you can keep it under wraps, but going shirtless or baring your back in a bathing suit puts the pimples on full display. If you’re wondering how to get rid of back acne, John Minni, DO, a board-certified dermatologist at Water’s Edge Dermatology, has answers.
Many of the same treatments that control facial acne can also be effective for back acne, but you’ll need to see your dermatologist if over-the-counter treatments don’t do the trick. You may want to make some lifestyle changes, too.
What causes back acne?
“The causes of facial and back acne — oil, dead skin flakes and bacteria — are the same,” said Dr. Minni. “But there are several other triggers of back acne that people need to be aware of, such as wearing tight-fitting clothes.”
These are the culprits that can lead to overproduction of oil and/or the growth of bacteria in pores.
Genetics
Genes play a major role in whether you get acne and where it develops. If you have back acne, chances are someone else in your family had it, too.
Hormones
Hormones can contribute to back acne, including female back acne. Women may get back acne in the week before their period starts, when they’re pregnant or when they’re in perimenopause or menopause. But men are more likely to get back acne than women.
“Testosterone stimulates the sebaceous glands to produce more oil, and there are a lot of sebaceous glands on the back, particularly the upper back,” Dr. Minni explained.
Sweat and friction
Wearing tight clothing, protective sports padding or a backpack can trap sweat and create friction that leads to bacne or makes existing bacne worse. The longer you let the sweat sit before showering, the bigger the problem.
Long hair
People with long hair may develop back acne, as well as acne on the back of the neck, from the hair care products they use, according to Dr. Minni.
“If you’re using heavy products such as deep conditioners and hair oils, these can be transferred from your hair to your upper back and cause acne.”
Medications
In some cases, back acne is a side effect of medication. Oral and topical steroids and certain cancer medications, for example, can trigger back acne in some people.
Types of back acne
Any type of acne can develop on the back, including whiteheads, blackheads, red bumps, pus-filled pimples, hard nodules and deep, painful cysts. You may have just one type of bacne or a combination of types. The upper back and shoulders are the most common sites, but some people develop acne all over their back and torso.
Back acne can be mild, severe or somewhere in between, and it may not match the severity of your facial acne. “You can have terrible back acne but mild facial acne and vice versa,” said Dr. Minni.
How to get rid of back acne: The best back acne treatment
Many of the same products you use to treat facial acne are also recommended for back acne, but treating back acne is less successful overall, according to Dr. Minni. That may be due to the challenge of applying topical treatments to your own back, as well as the fact that body acne can be deeper and more stubborn than facial acne.
You may not be able to get rid of back acne on your own unless it’s mild. If you have moderate to severe back acne, or you’ve been using over-the-counter products for eight weeks with no improvement, see your dermatologist.
Over-the-counter back acne treatments
- Acne-fighting cleanser. Choose one that contains salicylic acid or sulfur. (Dr. Minni cautions that benzoyl peroxide can bleach clothing.) Salicylic acid reduces acne and exfoliates the skin, keeping the pores clear of oil and dead skin. Sulfur reduces oiliness, prevents pore blockages and fights bacteria. An over-the-counter sulfur wash may be effective as a back acne wash, but if it doesn’t help enough, your dermatologist may recommend a prescription-strength version.
- Azelaic acid. Available in gels, foams and cream foams, azelaic acid clears pores, calms inflammation and encourages faster healing of acne with less scarring. You can find azelaic acid products at your local pharmacy, but your dermatologist may recommend a prescription-strength version if they don’t deliver results.
- Adapalene (Differin). This OTC retinoid helps unclog pores and prevents new acne from forming. It also improves skin’s texture and tone. Adapalene is often used in combination with benzoyl peroxide for maximum effectiveness, but it also works when used alone.
Prescription back acne treatments
- Topical retinoids. Prescription-strength retinoids, including tazarotene (Tazorac) and tretinoin (Retin-A), fight acne in the same ways adapalene does but they are stronger and more likely to work for moderate to severe back acne.
- Oral or topical antibiotics. Antibiotics slow or stop the growth of bacteria that infiltrate clogged pores. “People might hesitate to take oral antibiotics, but when prescribed for acne, the dose is so low that it doesn’t contribute to antibiotic resistance,” Dr. Minni noted.
- Isotretinoin. Known by its former brand name, Accutane, isotretinoin may be recommended if your back acne doesn’t respond well to antibiotics or you have deep, painful acne cysts and nodules on your back. This oral medication can have serious side effects (liver damage, pregnancy risks such as severe birth defects and miscarriage), so you’ll be closely monitored by your dermatologist while you take it.
In-office procedures
Treatments such as chemical peels and light or laser therapy can fight back acne. Chemical peels work by preventing clogged pores. Light or laser therapy targets bacteria that contributes to acne.
How to prevent back acne
Back acne can be hard to prevent if you’re genetically prone to develop it or if it’s triggered by hormones, but these steps may help you keep the worst of it at bay.
- Be gentle. Using harsh scrubs or astringents or tools such as loofahs or back brushes can make back acne worse.
- Shower ASAP after you sweat. If you can’t, use oil-free cleansing wipes to remove sweat.
- Avoid fabrics and bags that trap sweat. Wear loose clothes made of breathable cotton or sweat-wicking material and wash them after each wearing. If you use a backpack, consider switching to a shoulder bag or duffle.
- Cover up in the sun. Contrary to popular belief, sun exposure isn’t good for acne. When the sun’s UV rays dehydrate the skin, it responds by producing even more oil, leading to breakouts.
- Don’t pick. Popping pimples damages the skin and can cause scars.
- Use clean linens and towels. Wash your bedding and towels regularly so bacteria doesn’t build up on them and transfer back to your skin. Always use a fresh towel after showering.
- Tweak your hair care routine. In the shower, wash and condition your hair first, then wash your body so the hair care products get washed away. If you have long hair, wear it up when you exercise so oil and dirt don’t transfer to your skin.
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Does Stress Cause Acne?
Medical Review By: Dr. John Minni
Pimples have a way of showing up at the worst possible time. Days or hours before a wedding, a reunion, a hot date, or a big presentation at work, a big fat blemish (or two, or three) appears, giving you yet another reason to feel stressed.
But does stress actually cause acne? Not exactly.
“There are several causes of acne, but stress isn’t one of them,” said John Minni, DO, a board-certified dermatologist at Water’s Edge Dermatology. “If you already have acne, however, stress can make it more severe.”
The stress-acne connection
Genetics and fluctuating levels of androgen hormones during puberty, menstruation, pregnancy, and menopause are two main factors that set the stage for acne. Taking certain medications, such as birth control pills, lithium, and corticosteroids, can also make people susceptible to acne.
Stress won’t give you acne if you’re not already predisposed to it, but it can make acne worse by causing levels of certain hormones to temporarily increase.
“When your fight-or-flight response is activated, the body releases stress hormones, such as cortisol and androgens,” Dr. Minni explained. “These hormones increase your skin’s oil production, which can exacerbate acne.”
Stress, anxiety, and fear might also worsen acne by triggering the production of cytokines, tiny proteins that stoke inflammation, including inflammation of the area around sebaceous glands, the glands that produce oil.
Stress-related disruptions in healthy habits play a role, too. “When you’re anxious, you may not sleep or eat as well as you normally do, which can worsen acne,” Dr. Minni said.
Some people turn to smoking, which is linked to an increase in blemishes. Others pick at their skin when they’re stressed, which can make blemishes more irritated and inflamed.
How to prevent stress-related acne breakouts
You can’t avoid stress altogether, but if you’re prone to acne, you can take steps to limit the effects stress has on your skin.
Develop a stress-relief habit
Dr. Minni encourages patients to embrace practices that relieve stress, whether it’s regular exercise or relaxation techniques such as yoga, meditation, or deep breathing, all of which can lower cortisol levels.
Follow an acne diet plan
There is no acne diet per se. But research suggests there are some foods that cause acne, or at least foods that make breakouts more likely in certain people. And they are some of the same foods we tend to “stress eat.”
“When people are stressed, they tend to eat more processed and sugary foods, which can increase inflammation and oil production,” said Dr. Minni. Studies suggest that swapping high-glycemic foods (think white bread, white rice, cookies and soda) for low-glycemic ones (think fruits, vegetables, beans and whole-cut oats) can make acne less severe.
Pre-plan for an important event
Finally, if you have an important event coming up and you’re determined to avoid stress-related acne flares, talk to your dermatologist.
“Certain treatments can be used temporarily to head off stress acne that doesn’t require any downtime, such as anti-inflammatory medications, gentle facials, and light therapy,” said Dr. Minni.
“For an event such as a wedding or the prom, where your appearance is particularly important, your dermatologist may recommend something stronger, such as low-dose steroids, to help you look your best.”
Contact Our Acne Dermatologists at Water's Edge Dermatology
Article Written By: Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Medical Review By: Dr. John Minni
Is Sun Good for Acne?
If you’re constantly battling pimples due to acne, it’s tempting to try just about anything to get rid of them. Some people believe lying out in the sun will help. The thinking goes that sunlight will dry out the oil in the skin and/or prevent oil production, resulting in clearer skin.
Sounds logical, right? After all, excessive oil production often plays a role in acne development, along with other factors such as bacteria and hormone imbalances. But in fact, the dehydrating effect the sun has on the skin ultimately does more harm than good, said Sydney VanHoose, a board-certified advanced practice registered nurse at Water’s Edge Dermatology.
“Sitting in the sun can make it seem like your acne is improving at first, but it leads to more breakouts later,” said VanHoose.
What’s more, if you don’t use sunscreen or cover up with protective clothing when you’re outdoors, you’re exposing yourself to UV rays that could make other complexion issues worse, and even lead to skin cancer.
How the sun triggers breakouts
“After you’ve been in the sun, the epidermis [the top layer of skin] starts to dry and thicken,” VanHoose explained. “When this happens, your body responds by producing even more oil to compensate for what was lost – and that can lead to more breakouts.”
This effect doesn’t occur immediately, which may be why people don’t realize the connection between sunlight and worsening acne. Another source of confusion is the fact that dermatologists sometimes recommend light therapy to treat acne; however, the blue light used in this FDA-approved treatment is very different from the sun’s rays. It kills acne-causing bacteria (P. acnes) without damaging the skin the way UV light does. Sunlight does not kill P. acnes.
Why people think the sun helps
A day, weekend or week in the sun can indeed make a difference temporarily, but not for the reasons people may think. If you get a tan, for instance, that can make red pimples stand out less. The stress-reducing effects of a vacation can also help, since stress is known to exacerbate acne.
A shortsighted trade-off
Even if sun worshipping did somehow lead to a clearer complexion, the other risks it poses to your skin simply aren’t worth it.
"Exposing acne to UV rays without any protection leads to an increased risk of scarring and hyperpigmentation," VanHoose said. "So, while people may think their complexion looks better when they tan, the trade-off is that they’re going to end up with more marks and dark spots, and possibly skin cancer, in the future."
Sun damage caused by unprotected sun exposure can also lead to premature skin aging and wrinkles. "A lot of people who have acne also want to treat fine lines on their face, and the sun’s not going to help with that, it’s going to make it worse," said VanHoose.
Even short bouts of sun exposure contribute to skin damage, so it’s important to wear a broad-spectrum, water resistant sunscreen with an SPF of at least 30 every day. Worried sunscreen will make your face look greasier or cause more breakouts? Read the label and find a product that is oil free and noncomedogenic.
Professional help for clear, beautiful skin
If you feel like you’ve tried everything to clear your complexion and nothing is working, see a dermatologist. “It’s best to get in the office, get a skin exam and have the dermatologist develop a targeted treatment plan that’s personalized for you,” VanHoose said.
A bonus: The dermatologist can recommend or prescribe products that can make your skin clearer and smoother, now and later in life. Retinoids, for example, not only unclog pores but help reduce the look of fine lines.
As VanHoose put it, "You’re going to be pretreating your skin for the future."
Written by Jessica Brown is a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation, and many more.
How to Get Rid of Acne Scars
Acne is double trouble: First there's the ugly blemishes. Then, in many cases, there are the scars that result. If you’re wondering whether it’s possible to get rid of acne scars, or at least make them less noticeable, the answer is yes.
The best acne scar treatment depends on your skin tone and the type of acne scars you have. Some acne scars are elevated, but most are depressed (indented). These are known as atrophic scars.
Common types of atrophic acne scars include:
| Ice pick scars — these are very small and deep, like the mark an ice pick would make | 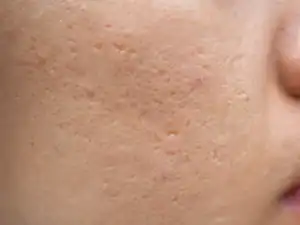 |
| Boxcar scars — these are wide, box-like depressions with distinct edges | 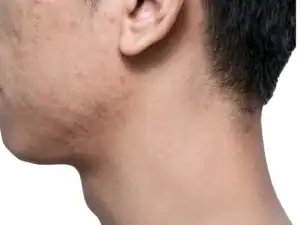 |
| Rolling scars — these have sloped edges and give the skin a wavy texture; they can be smoothed out if the skin is stretched | 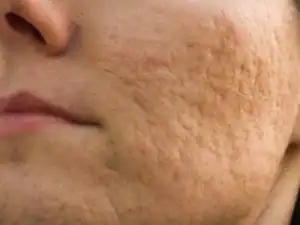 |
Acne scar treatments include fractional CO2 laser therapy, microneedling, subcision, chemical peels, dermabrasion, dermal fillers and mini-excision. Some treatments aren’t ideal for skin of color because they pose a risk of hyperpigmentation (dark patches) or changes in skin color. For the best results, you may need a combination of different treatments. A dermatologist can determine the appropriate treatment plan for your acne scars.
Remember, picking at acne blemishes can increase the chances of scarring, so if you’re guilty of that habit, do your best to break it.
Fractional CO2 laser therapy
Fractional CO2 (carbon dioxide) laser therapy, a new twist on CO2 lasering, has revolutionized the treatment of acne scars. The laser makes microscopic perforations in the skin, and as these wounds heal, new collagen is produced under the skin, which can smooth out the surface and raise depressed scars. Other benefits include tighter skin and a brighter complexion. “Fractional” means the beams of light are split into thousands of columns so that only a fraction of the targeted skin is perforated, leaving unperforated areas between the “dots.” This speeds healing and lowers the risk of complications.
Prior to beginning this procedure, the provider injects or applies a local or topical anesthetic. Following the treatment, your skin will look red and possibly swollen and may flake for a week or more. You won’t see full results for at least three months. People with very dark skin may not be good candidates for this treatment.
Fractional CO2 laser therapy may be combined with chemical peels, subcision, microneedling, dermal fillers and/or platelet-rich plasma (PRP) therapy. In PRP therapy, plasma is taken from your own blood and injected into your skin. Proteins in the plasma stimulate collagen-producing cells in the skin to produce more collagen. One study found that fractional CO2 lasering combined with PRP produced better, faster results for atrophic acne scars than lasering alone.
Microneedling
Microneedling is all the rage these days for reducing the look of wrinkles, crow's feet and enlarged pores, but microneedling for acne scars isn’t new. In microneedling, a dermaroller (a hand-held device shaped like a mini paint roller and covered with small shallow needles) is used to make tiny punctures in the skin. The body responds by filling the wounds with collagen and elastin, which makes the skin look smoother and tighter. You’ll see continued improvement over the course of weeks and months as the collagen and elastin do their work.
Microneedling is safe for multiple skin types and tones. The procedure is mostly painless. You might have some mild swelling and bruising. Typically, several treatment sessions are needed.
For faster results, perhaps with fewer treatments, there’s microneedling with radiofrequency, aka microneedling RF, in which heat is applied between the needles. This boosts the production of collagen and elastin. Microneedling RF can be further enhanced by applying platelet rich plasma (PRP) to the skin after the procedure. PRP, derived from your own blood (which means you’ll need to have blood drawn), contains proteins that help the skin repair itself.
Subcision
Rolling or boxcar acne scars, which often have fibrous attachments anchoring the base of the scar to underlying tissue, are excellent candidates for subcision. In subcision, a specialized hypodermic needle is inserted through the scar and used to release the base. This allows for the generation of new collagen beneath the scar, which lifts and smooths the surface.
“The procedure generally takes 15-30 minutes," said Dr. Christopher Spock, a dermatologist with Water’s Edge Dermatology. “Patients typically require multiple treatments, usually spaced six to eight weeks apart. Topical numbing gel and injectable anesthesia are used to keep them very comfortable throughout the procedure.”
Chemical peel
In a chemical peel, acid is applied to the skin to make it smoother and softer while minimizing the look of fine lines and brown spots. There are two types of chemical peels for acne scars.
In the CROSS technique, which works well for ice pick and boxcar scars, a high concentration of trichloroacetic acid (TCA) is placed in the scar. Wound healing triggers the production of collagen, which smooths the skin’s surface.
The second chemical peel approach is a total face chemical peel, which uses a lower concentration of TCA, or Jessner’s solution, salicylic acid or glycolic acid, to remove the top layer of skin, which smooths the surface. This type of chemical peel also stimulates the production of skin-rejuvenating collagen.
Generally speaking, superficial chemical peels (which affect only the top layer of skin) are safe for all skin types, including dark skin. Side effects include a slight burning sensation, redness and possibly some swelling.
Dermabrasion
In dermabrasion (not to be confused with microdermabrasion), the provider uses a small, hand-held medical-grade sander to sand the outer layers of skin and precisely contour underlying scars. You’ll be given a local anesthetic beforehand. Following the procedure, you may have swelling and feel some pain (usually minimal). The skin usually heals in seven to 10 days, though pinkness or redness may last for up to three months. Multiple sessions are often needed.
Dermabrasion may not be the best choice for people with darker skin.
Dermal fillers
Dermal fillers such as Restylane, Juvederm or Belotero can be injected under depressed acne scars to lift the indented skin, making skin look smoother immediately. The results last for many months. Some of the improvement may be permanent.
Fillers make the most sense when acne scars are isolated. They work especially well on rolling scars. They may not work as well for ice pick scars.
Mini-excision
Raised scars and scars that are very deep are often best removed surgically. With mini excision, the scar is cut out completely and the skin edges are stitched together. The scar that results, in the form of a fine line, is much less visible than the original acne scar — and it can be minimized with other scar treatments if you want even smoother skin.
Article Written By: Marianne Wait, an award-winning health and wellness writer based in New Jersey.
Medically Reviewed By: Christopher Spock, MD
Study Shows Tretinoin Top Choice for Anti-aging
March 8 is International Women’s Day, and since 1911, it has been a day to celebrate women around the world. We want to encourage everyone to make a positive difference for all of the women and girls in your life every day. Your Water’s Edge team is committed to celebrating you and delivering the latest news in skin health so you can enjoy a lifetime of looking as young as you feel.
Our number one recommendation for skin protection is to be sure you and your family are using sunscreen to protect skin from the damaging rays of the sun. Regular use of sunscreen is also the number one anti-aging recommendation. Be sure you begin using sunscreen as early in life as possible. To prevent visible signs of aging that already exist, dermatologists recommend a retinol product to stimulate skin cell turnover and collagen production while exfoliating the top layers of skin to reveal fresher, younger-looking skin underneath.
Unlike many retinol skincare products on the market, Tretinoin is approved by the FDA for anti-aging and has become the gold standard for anti-aging skincare. Studies have shown that Tretinoin increases collagen and reduces fine lines and wrinkles by speeding cell turnover. These studies have also confirmed that Tretinoin brightens skin and smooths skin’s texture. It is also effective in reducing hyperpigmentation, skin discoloration and the formation of acne.
When compared with over-the-counter retinoid products, Tretinoin works faster and delivers more powerful results because it contains 20 times the retinol concentration allowed by the FDA for non-prescription, over-the-counter formulations. It is considered a medical grade prescription topical treatment that supports skin becoming stronger with a tighter and firmer appearance.
A recent study of the comparative effects of retinol and retinoic acid in the Journal of Cosmetic Dermatology looked at the efficacy of a retinol formulation for improving skin’s appearance. Four weeks of retinol treatments showed an increase in epidermal thickness, collagen production and a significant reduction in facial wrinkles.
The study results also demonstrate that topical application of retinol affects both cellular and molecular properties in the epidermis and dermis.
Tretinoin is Water’s Edge Dermatology’s most recommended product because it delivers results. Water’s Edge Tretinoin is available by prescription in three strengths with 0.025% retinoic acid; 0.05% retinoic acid and 0.1% retinoic acid.
Many dermatologists recommend that anyone over 30 begin using Tretinoin in order to prevent the visible signs of aging. Our Water’s Edge clients love Tretinoin because they are seeing positive results in healthier and more youthful looking skin. You may notice results in a few as four weeks, and when using Tretinoin, remember to always wear sunscreen to get the full benefit and protect your skin from the sun.
Click here to make an appointment today at Water’s Edge Dermatology and learn more about how Tretinoin can help you look as young as you feel. Also, please share this blog with a friend and refer them to Water’s Edge Dermatology.
Top 5 Causes of Children's School Year Skin Problems
When summer officially ends every late September, the somewhat stressful “Back-to-School” season is also pretty much over with – whew! The question is, did shopping for school supplies and other preparations also leave you well-prepared for dealing with inevitable school year skin problems?
Below are 5 of the most common causes of skin problems among schoolchildren, plus some practical skincare tips on how to prevent or treat them.
Stress
It’s remarkable how much stress affects the skin. Various rashes and acne are commonly caused by stress. So what can you do to help minimize the impact of stress on your children's skin? Find the right tools and techniques to keep their stress levels low (easier said than done, but think communication, exercise & relaxation). Ensure they gently wash their face twice daily with a mild, natural cleanser and warm rather than hot water. And get them to use a hypoallergenic, lightweight moisturizer (with SPF 30 or higher sun protection) daily.
Hormones
Hormones can play a huge role in causing acne for teens, and for an increasing numbers of "tweens" too. Getting your schoolkids into a consistent daily facial cleansing and skincare routine is extremely important. Visiting a dermatologist for the right acne treatment will be warranted in some cases. In extreme instances, you may also want to ask your family physician if hormone therapy is worth consideration.
Sweat
Let’s face it. Here in South Florida, everyone sweats, which can cause rashes and acne breakouts. Training your children to seek shade outside and stay as dry as possible can help. Same with washing off sweat as soon as possible. Consider adding gentle, individually wrapped facial wipes, a lightweight, comfy cap or hat and a soft, absorbent washcloth or bandana to their daily backpack load. But remember to put that bandana in a baggie to keep it clean, and replace with a clean, dry one each day!
Sports
Autumn sports such as football can cause their own set of skin conditions. In Florida, there’s still the sun and heat causing heavy sweating. And sports helmets can cause folliculitis (inflammation of hair follicles). Washing the face immediately after sports activity and cleaning helmet pads with rubbing alcohol are good preventive measures. Some sports uniforms and gear can also cause allergic reactions to some kids. If skin irritations develop in weeks after donning uniforms, a trip to your nearest Water’s Edge Dermatology office is in order.
Shoes/Clothing
Switching from summer’s tank-tops, shorts, and flip-flops to shoes, sneakers, and school uniforms can trigger common skin conditions, such as athlete’s foot. Breathable socks that wick away moisture from damp feet and over-the-counter foot powders that do the same can help prevent such fungal skin infections. New school uniforms should always be washed before first wearing, and if possible, given a day of “test-wearing” to identify any possible irritation or allergic reaction.
Of course, getting the kids on board with a program that addresses the 5 issues above can be…challenging. Explain to them that getting and keeping the clear skin they crave is the goal, the reason for all the extra efforts. Putting sticky notes on bathroom/bedroom mirrors at home with gentle and/or humorous reminders can also help. And if/when needed, virtually all of our dermatology providers specialize in pediatric dermatology as well as adult skincare.
For questions on common school year skin conditions affecting children, such as skin rashes, skin infections and head lice, please contact Water’s Edge Dermatology for an appointment with one of our practitioners by calling your local office, or toll-free at (877) 900-3223. You can also request an appointment online.
Here's to you and your children having a happy, healthy school year!
What Your Acne Might Be Telling You
If you're an adult with acne, don't worry. You're not alone. According to recent statistics, nearly 85% of all adults get acne at some point in their lives, whether it's on the face, chest, or other parts of their body. In the U.S. alone, between 40 and 50 million people are currently dealing with some form of acne.
When one is dealing with acne, the best thing to do is to visit the local dermatologist to seek out the best skin care treatments for acne. However, that's not always the full picture to perfect skin. Rather, having good skin care habits and overall health will prevent you from experiencing unwanted blemishes. So if you have acne, your skin may be trying to tell you something.
Here's what your acne-prone skin might be trying to say:
You're Dehydrated
For those who are acne-prone, dehydration can exacerbate skin problems. According to Fix.com, one of the symptoms of dehydration is dry skin. When your skin lacks moisture, your body will attempt to overcompensate by producing more oils to moisturize your dry skin, furthermore causing breakouts.
Your Diet is Off
Studies show that highly processed foods with a high glycemic index and tons of carbohydrates can easily cause acne and inflammation in many individuals. Dairy and sugar are also common causes of inflammation and breakouts. If you're experiencing a lot of breakouts, it may be time to eat more fruits and vegetables.
You're Tired
If you're not getting all 40 winks, then you may be experiencing acne. When you don't get enough sleep, your body isn't as able to increase blood flow to the skin. It also messes with your body's ability to create new collagen overnight. Additionally, not getting enough sleep can mess with your stress levels, which can also lead to acne.
You Need to Lay off the Cocktails
As you may already know, drinking is extremely bad for your skin. Not only can it dry your skin out, leading to the production of acne-causing oils, but it can also lead to other poor habits, such as many of the ones listed above.
A positive change in life habits, combined with regular visits to your local dermatologist and the best acne treatment possible can help to make your skin healthy and glowing. Of course, you can always ask a dermatologist if you ever need any counsel or guidance.